|
SHUNTING |
|
Intra-arterial shunts provide a bloodless operative field while providing blood flow to the distal myocardium. Shunting can potentially eliminate the need for ischemic preconditioning and prevent dysrhythmia and hemodynamic compromise. In addition, shunts act as a suture guide by preventing the back wall of the arteriotomy from being accidentally included in the suture. Another benefit of shunts is that they can be used as a "poor man's" graft patency test – when the shunt is extracted without resistance, patency is confirmed.21 Shunt efficacy can be demonstrated by observing EKG changes
after insertion of the shunt. In the clinical example illustrated
in Figure 10, a large RCA with a tight proximal stenosis was
occluded. Marked EKG changes were noted after three minutes
of a test occlusion. The artery was then reperfused. After reperfusion,
the RCA was occluded again, opened, and the aortocoronary shunt
was inserted. The EKG after shunt insertion was unchanged from
baseline.22 |
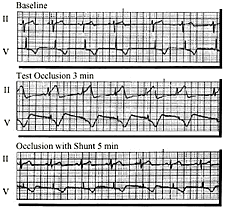 Figure 10. EKG at baseline, during a test occlusion and during occlusion with an aortocoronary shunt in place |
| "The aortocoronary shunt, by reducing regional myocardial ischemia, has enhanced hemodynamic stability during Octopus coronary artery bypass grafting, thereby facilitating an unhurried, precise anastomosis." 22 -Carl E. Arentzen, M.D. Surgeon |
|
Shunts can be classified in three different categories
|
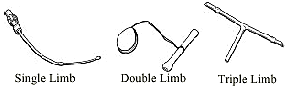
Figure 11. Single-, double-, and triple-limb shunts |
| "I am now using intraluminal shunts in approximately 50% of my cases. In large LADs with subtotal stenosis, shunting may prevent unwanted ST changes and hemodynamic instability. In large RCA arteries with only moderate proximal stenosis, one may encounter bradyarrhythmias and/or hypotension during test occlusion. Intraluminal shunts have reportedly reversed these hemodynamic changes. I do not want to place myself 'under the gun,' trying to rapidly complete an anastomosis while the hemodynamic condition is deteriorating."13 -James C. Hart, M.D. |